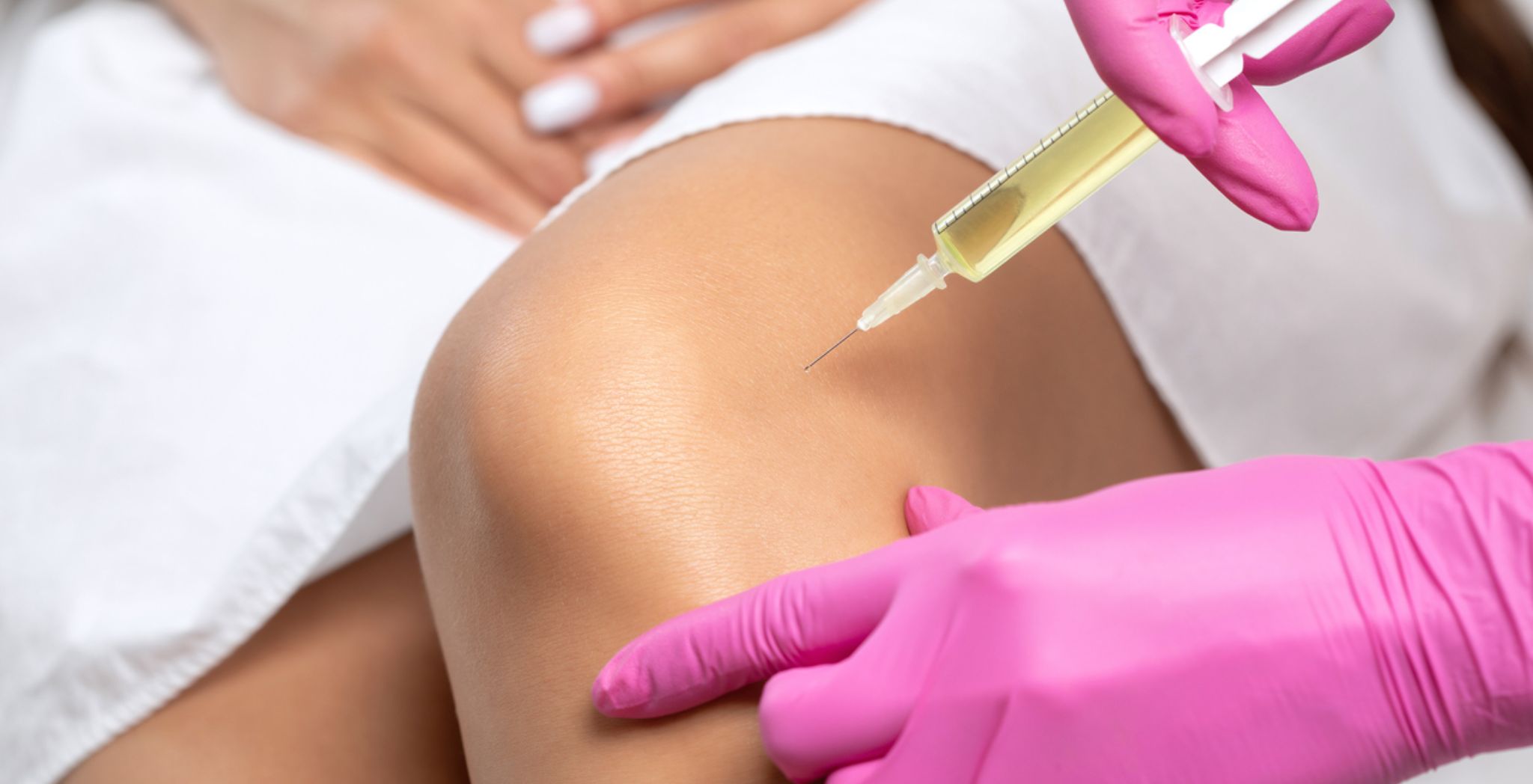
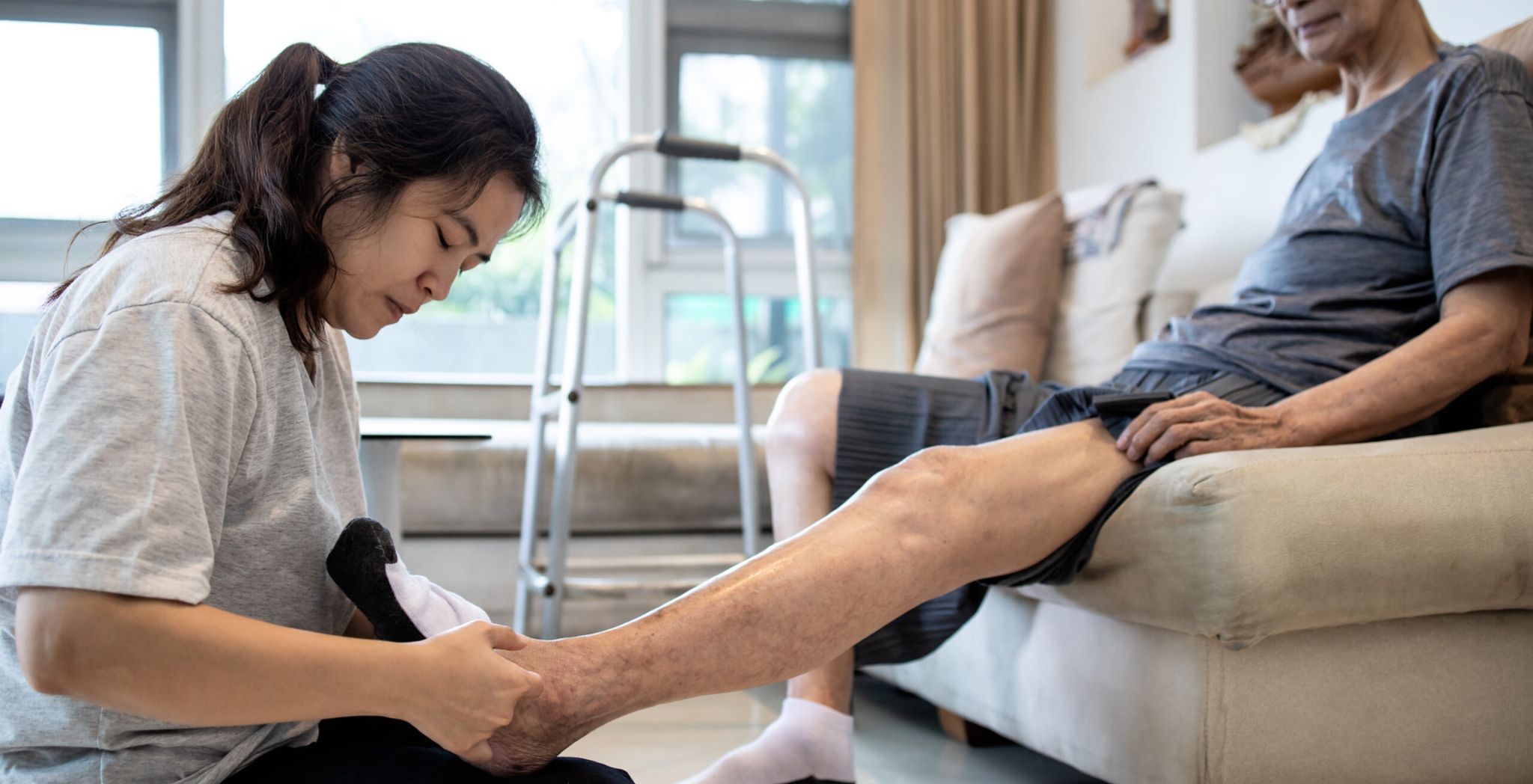
Introduction
Every athlete, weekend warrior, or active person knows the frustration of dealing with pain that just won’t go away. Whether it’s a nagging knee, a worn-out hip, or a shoulder that never quite healed right, chronic musculoskeletal injuries can steal the joy from the activities you love most.
For decades, the standard answer was rest, physical therapy, pain medications, or eventually surgery. But today, a growing field called regenerative sports medicine is changing the conversation entirely. Instead of simply managing pain or replacing joints, regenerative medicine asks a much more exciting question: what if we could help the body repair itself?
This blog breaks down everything you need to know about regenerative sports medicine, what it is, how it works, its key benefits, and who stands to gain the most from it. Whether you are dealing with hip pain, joint degeneration, or chronic sports injuries, this guide will give you a clear picture of what modern medicine now makes possible.
What Is Regenerative Sports Medicine?
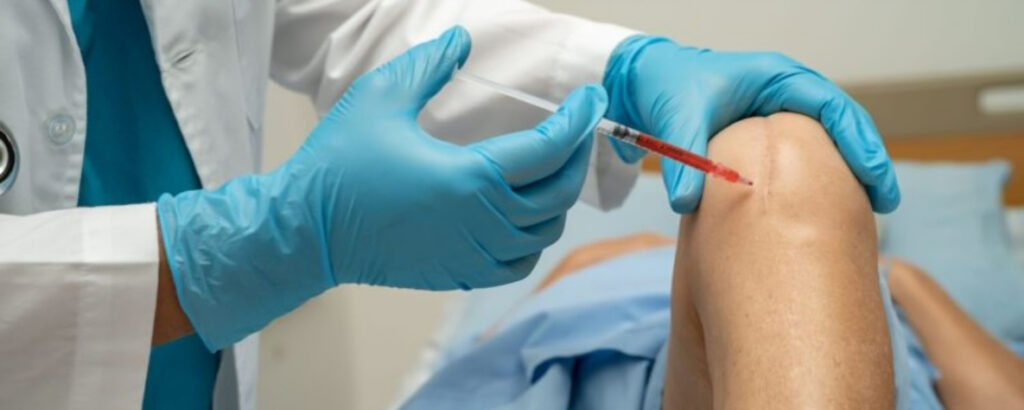
Regenerative sports medicine is a branch of medicine that uses the body’s own natural healing mechanisms or lab-assisted biological tools to repair damaged tissues like cartilage, tendons, ligaments, and bones. Rather than cutting out or replacing a damaged body part, regenerative treatments focus on stimulating the body to heal from the inside out.
The field sits at the intersection of sports medicine, orthopedics, and cutting-edge biology. Doctors who practice it draw on a range of therapies, from platelet-rich plasma (PRP) injections to stem cell therapy for joints. The underlying philosophy is simple: the human body has remarkable self-repair capabilities, and regenerative medicine is about unlocking and amplifying those capabilities.
This approach is especially appealing for athletes and physically active individuals who want to avoid surgery, reduce downtime, and get back to performing at their best as quickly and safely as possible.
How Regenerative Sports Medicine Works
To understand how regenerative sports medicine works, it helps to understand why injuries become chronic in the first place. Tissues like cartilage and tendons have poor blood supply. When they are damaged, the healing signals that normally rush to an injury site simply don’t arrive in adequate numbers. The result is slow, incomplete, or scar-heavy healing that leaves you with stiffness, weakness, and ongoing pain.
Regenerative treatments work by delivering concentrated biological signals directly to the injury site. These signals may come in the form of growth factors, stem cells, or other cellular messengers. Once introduced to the damaged tissue, they trigger a cascade of repair activity, prompting cells to multiply, rebuild, and reorganize into healthy, functional tissue.
This is not a one-size-fits-all process. Depending on the injury, a doctor might recommend a single injection, a series of treatments, or a combination of therapies. The goal in every case is the same: real tissue repair, not just symptom relief.
Key Benefits of Regenerative Sports Medicine
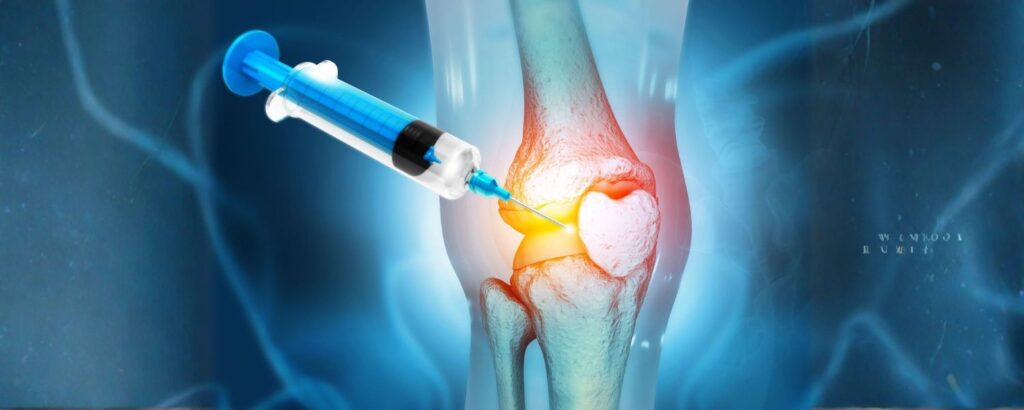
The benefits of regenerative sports medicine are wide-ranging, and they go well beyond simply reducing pain. Here is a closer look at what makes this field so promising.
Natural Healing Without Surgery: One of the biggest draws of regenerative sports medicine is its ability to promote genuine healing without putting a patient under the knife. Surgeries come with risks, such as anesthesia complications, infections, lengthy recovery periods, and the possibility that scar tissue will create new problems. Regenerative treatments, by contrast, are minimally invasive, typically involving little more than a targeted injection.
Reduced Recovery Time: Traditional surgical recovery can sideline an athlete for months. Regenerative treatments often allow patients to return to light activity within days and to full activity within weeks, depending on the severity of the injury and the type of treatment used.
Long-Lasting Results: Because regenerative therapies aim to repair the underlying tissue rather than just block pain signals, the results tend to be more durable. Patients who respond well to treatments like stem cell therapy for joints often report improvements that last for years.
Lower Risk of Side Effects: Since most regenerative treatments use biological material sourced from the patient’s own body, their own blood, fat, or bone marrow, the risk of allergic reactions or immune rejection is very low. This autologous approach makes regenerative medicine one of the safer options in modern orthopedics.
Reduced Dependence on Pain Medication: Chronic pain often leads to long-term reliance on anti-inflammatory drugs or opioids, both of which carry significant health risks. By addressing the root cause of pain through tissue repair, regenerative medicine can help patients significantly reduce or even eliminate their need for these medications.
Preservation of Natural Joint Structure: Joint replacement surgery, while sometimes necessary, permanently alters the body’s anatomy. Regenerative sports medicine prioritizes preserving the body’s natural structures, which is especially important for younger patients who may otherwise face multiple revision surgeries over a lifetime.
Common Treatments Used in Regenerative Sports Medicine
Several core treatments form the backbone of regenerative sports medicine today.
Platelet-Rich Plasma (PRP) Therapy: PRP is one of the most widely used regenerative treatments. It involves drawing a small amount of the patient’s blood, spinning it in a centrifuge to concentrate the platelets and growth factors, and then injecting this concentrated solution into the injured area. Platelets are rich in proteins that signal tissue repair, making PRP a powerful tool for treating tendon injuries, mild arthritis, and ligament damage.
Stem Cell Therapy: Stem cell therapy for joints involves harvesting stem cells, typically from the patient’s bone marrow or fatty tissue, and injecting them into damaged areas. Stem cells have the unique ability to differentiate into various types of tissue, meaning they can potentially become new cartilage, tendon, or bone cells depending on where they are placed. This makes them particularly valuable for conditions involving cartilage loss or joint degeneration.
Prolotherapy: Prolotherapy uses injections of an irritant solution, often a sugar-based compound, to provoke a controlled inflammatory response. This response stimulates the body’s repair mechanisms in connective tissues that have become chronically lax or damaged. It is commonly used for ligament injuries and lower back pain.
Bone Marrow Aspirate Concentrate (BMAC): BMAC is a more advanced form of cellular therapy that extracts a concentrate rich in stem cells and growth factors directly from the patient’s bone marrow. It is often used in more significant joint injuries and is considered a step up from standard PRP in terms of regenerative potential.
Conditions Treated with Regenerative Sports Medicine
Regenerative sports medicine is remarkably versatile. It has shown meaningful results across a wide range of conditions, including:
Osteoarthritis of the knee, hip, and shoulder; tendinopathies such as Achilles tendinitis and rotator cuff injuries; partial ligament tears, including ACL and MCL injuries; cartilage defects and early-stage chondral damage; plantar fasciitis; chronic lower back pain; labral tears of the hip; and meniscus injuries.
Each of these conditions involves some degree of tissue breakdown that the body has struggled to repair on its own. Regenerative treatments step in to provide the biological boost needed to restart or accelerate that healing process.
Stem Cell Therapy for Joints and Hips Explained
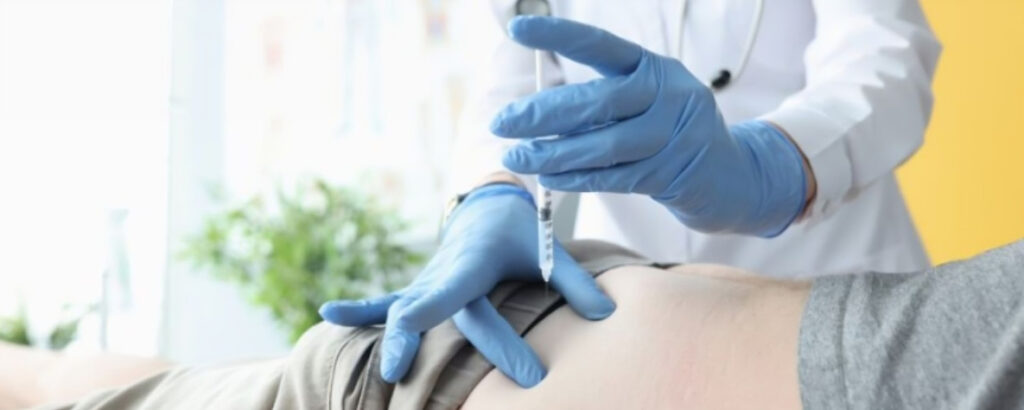
Among all regenerative treatments, stem cell therapy for joints and specifically stem cell therapy for hips has attracted particular attention. The hip is a high-load joint that bears the full weight of the body during nearly every activity. When hip cartilage degrades, whether from injury, overuse, or age, the resulting pain can be debilitating.
Hip pain treatment has historically been limited to cortisone injections, physical therapy, and eventually, total hip replacement. Stem cell therapy offers a middle path. By injecting concentrated stem cells directly into the hip joint, doctors aim to rebuild the deteriorating cartilage, reduce inflammation, and restore more normal joint function.
Early clinical research and patient outcomes have been encouraging. Many individuals who received stem cell therapy for their hips have reported significant reductions in pain and improvements in mobility, sometimes avoiding hip replacement surgery for several years or indefinitely.
The procedure itself is typically performed under imaging guidance to ensure precision. Recovery is generally much faster than surgical alternatives, and many patients notice gradual improvements over the months following treatment as the newly introduced cells integrate and begin their repair work.
Cellular Therapy for Pain Management
Cellular therapy for pain is about more than just sports injuries. Chronic pain from degenerative conditions affects millions of people who are not athletes, including older adults with joint disease, individuals with autoimmune conditions affecting the joints, and people recovering from traumatic injuries.
Cellular therapy works by modulating the inflammatory environment within damaged tissues. Many forms of chronic pain are sustained by ongoing, low-grade inflammation. Stem cells and other cellular agents can release anti-inflammatory molecules that calm this environment, breaking the cycle of chronic inflammation and giving damaged tissue the space to heal.
This dual action, both repairing tissue and reducing inflammation, makes cellular therapy for pain one of the most exciting developments in non-surgical pain management today.
Who Can Benefit from Regenerative Sports Medicine?
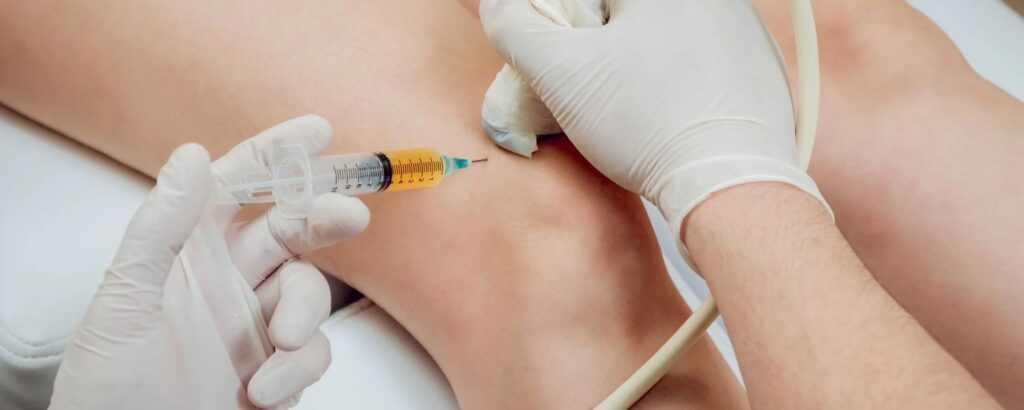
Regenerative sports medicine is not exclusively for elite athletes. A wide range of people are good candidates, including recreational athletes dealing with persistent joint or tendon injuries; middle-aged individuals with early to moderate osteoarthritis who want to delay or avoid joint replacement; older adults seeking to maintain mobility and independence; and anyone who has not found lasting relief through conventional physical therapy or injections.
The ideal candidates maintain reasonable overall health, avoid advanced joint destruction, and commit to following rehabilitation protocols that support the regenerative process. A thorough evaluation by a qualified sports medicine or orthopedic physician is always the first step to determine whether regenerative therapy is appropriate for a specific condition.
Conclusion
Regenerative sports medicine represents a genuine shift in how we think about healing. It moves us away from a model of simply managing pain or replacing worn-out parts, toward one that honors the body’s natural intelligence and works with it. From stem cell therapy for joints to cellular therapy for pain, the tools now available offer real hope to people who have been told surgery is their only option.
If you are living with hip pain, joint degeneration, or a chronic sports injury, exploring regenerative medicine with a qualified practitioner could be one of the most important steps you take toward a more active, pain-free life.
Frequently Asked Questions
1. What is regenerative sports medicine?
A. Regenerative sports medicine is a medical specialty that uses biologically active treatments such as PRP, stem cells, and other cellular therapies to repair damaged muscles, tendons, cartilage, and joints. It focuses on healing the root cause of injuries rather than just reducing symptoms.
2. How does stem cell therapy help joints?
A. Stem cell therapy for joints works by delivering concentrated stem cells directly into damaged joint tissue. These cells can differentiate into the specific tissue types needed for repair, rebuild cartilage, reduce inflammation, and stimulate the body’s natural healing response, often producing significant improvements in pain and function.
3. Is regenerative sports medicine effective for hip pain treatment?
A. Yes. Stem cell therapy for hips and PRP injections have both shown promising results for hip pain caused by osteoarthritis, labral tears, and cartilage damage. Many patients experience meaningful pain relief and improved mobility, and some have been able to avoid or significantly delay hip replacement surgery.
4. What conditions can be treated with cellular therapy for pain?
A. Cellular therapy for pain is used for a wide range of conditions, including osteoarthritis, tendinopathies, ligament injuries, cartilage defects, chronic lower back pain, and meniscus injuries. It is effective both for athletes recovering from sports injuries and for everyday individuals dealing with degenerative joint disease.
5. Who should consider regenerative sports medicine?
A. Anyone dealing with a chronic musculoskeletal injury, early to moderate joint degeneration, or persistent pain that has not responded adequately to conventional treatments may be a good candidate. A consultation with a regenerative medicine specialist will determine whether the approach is suitable based on the individual’s specific condition, overall health, and treatment goals.