Introduction
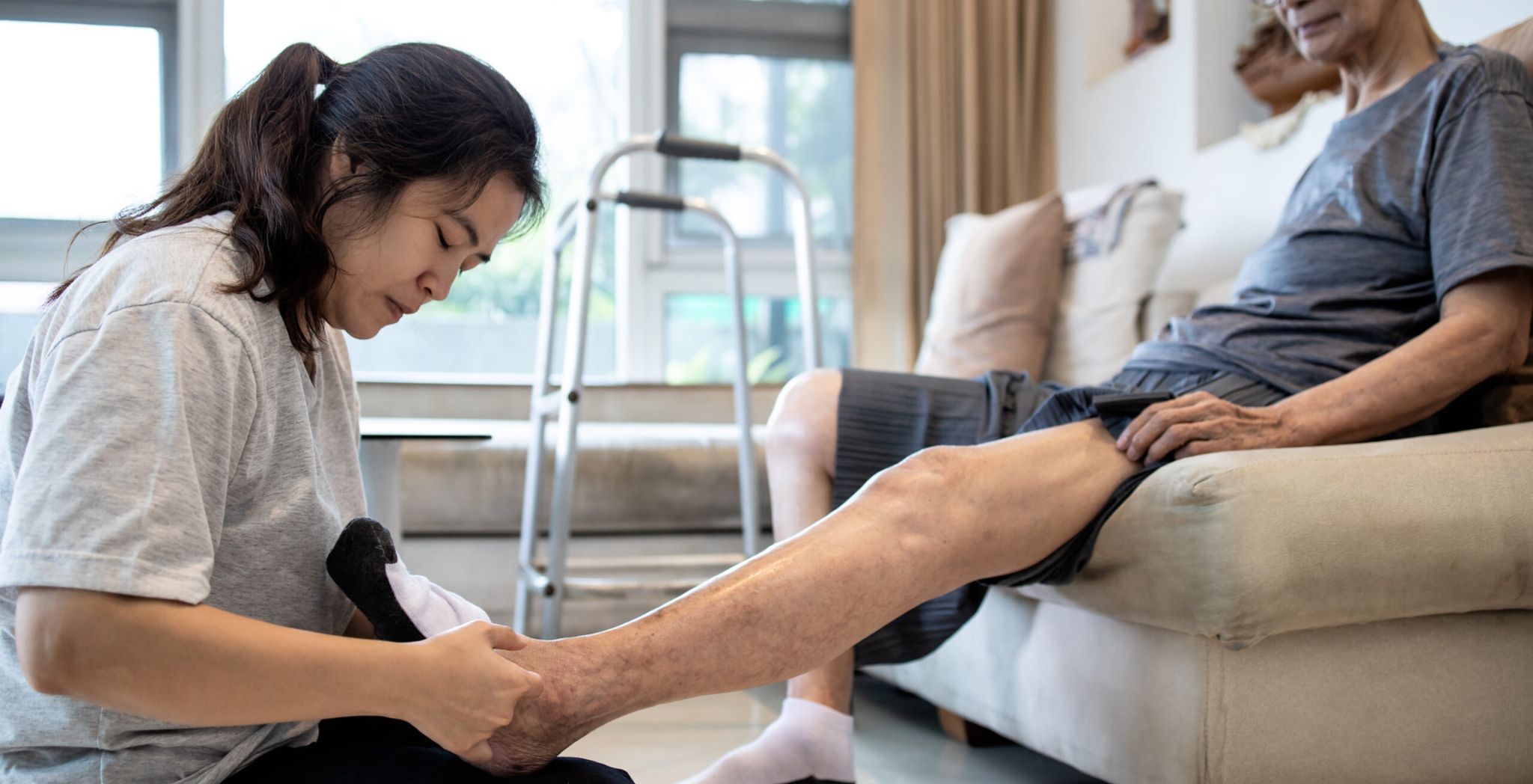
Every morning, millions of people wake up dreading the simple act of getting out of bed. Not because they’re lazy but because their joints make even basic movements feel like a battle. Whether it’s a stiff knee, an aching shoulder, or a lower back that protests every twist and bend, joint pain has a way of quietly shrinking your world.
You miss out on walks. Family outings are left behind. Activities that once brought joy get pushed aside. Over time, it’s not just the pain that wears you down, it’s the loss of independence, the frustration of being held back by your own body.
But here’s the good news: joint pain treatment has come a long way. From conventional therapies to cutting-edge regenerative medicine, there are real solutions available today that go beyond simply masking pain. This guide breaks everything down so you can understand your options and take the first step toward feeling better.
What Is Joint Pain?
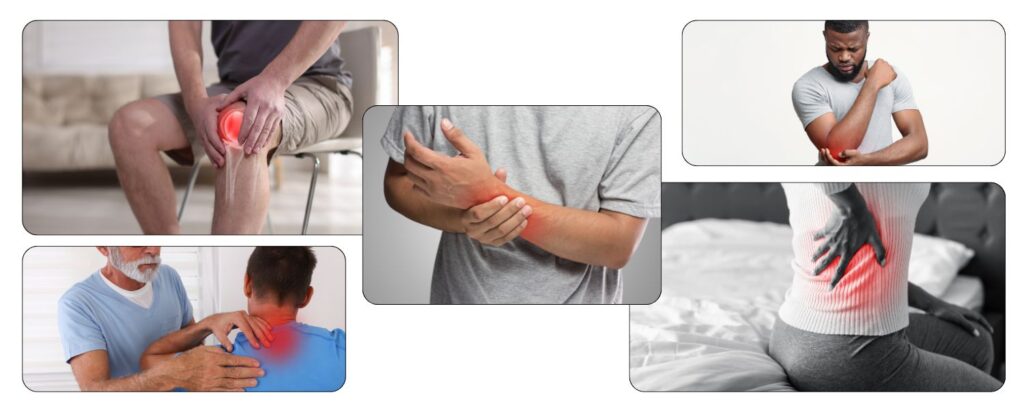
Joint pain refers to any discomfort, soreness, or inflammation that occurs where two bones meet. These meeting points, your joints are cushioned by cartilage, lubricated by fluid, and supported by tendons and ligaments. When any part of this system breaks down, pain follows.
The most commonly affected areas include:
Knees: Taking the full weight of your body with every step makes the knees particularly vulnerable. Osteoarthritis, ligament tears, and meniscus damage are frequent culprits.
Shoulders: A complex joint built for a wide range of motion, the shoulder is prone to rotator cuff injuries, tendinitis, and impingement syndromes.
Hips: Often damaged by arthritis or injury, hip joint pain can radiate down through the thigh and make walking painful.
Spine and Back: While technically a series of joints, the spine is frequently affected by disc deterioration, facet joint issues, and compression.
Hands, Wrists, and Ankles: These smaller joints are often hit hard by rheumatoid arthritis and repetitive strain.
Regardless of location, joint pain generally stems from one of a few root causes: physical injury, wear-and-tear (osteoarthritis), autoimmune conditions like rheumatoid arthritis, or inflammation triggered by lifestyle factors such as excess weight or poor posture.
The Benefits of Seeking Joint Pain Treatment
Some people try to push through joint pain, hoping it will go away on its own. Occasionally, it does. But when pain persists for weeks or starts affecting your daily routine, ignoring it typically makes things worse, not better.
Seeking timely joint pain treatment offers several meaningful benefits:
Pain Relief: The most immediate goal. Effective treatment brings down inflammation, calms nerve signals, and gives damaged tissue the chance to heal.
Improved Mobility: When pain drops, movement comes back. Patients who receive treatment often find they can walk farther, climb stairs, sleep better, and simply do more.
Slowed Progression: Left untreated, many joint conditions worsen over time. Early intervention can slow this process significantly.
Reduced Dependence on Medication: Many people rely on painkillers to get through the day. Proper joint care can reduce or even eliminate that need.
Better Quality of Life: This one is hard to quantify but easy to feel. When your body stops fighting you, everyday life becomes more enjoyable again.
Regenerative Medicine for Joint Pain
Traditional joint treatments, such as anti-inflammatory drugs, corticosteroid injections, and physical therapy, remain useful. But they often work by managing symptoms rather than addressing the underlying damage.
Regenerative medicine takes a different approach. Instead of simply reducing pain signals, it aims to help the body repair itself at a cellular level. This field has gained significant attention in recent years because of its potential to offer long-lasting results where conventional treatments fall short.
The two most widely used regenerative approaches for joint pain are stem cell therapy and platelet-rich plasma (PRP) therapy.
Platelet-Rich Plasma (PRP) Therapy works by drawing a small amount of the patient’s own blood, processing it to concentrate the growth factors found in platelets, and injecting that concentrated solution directly into the affected joint. These growth factors help stimulate healing, reduce inflammation, and encourage tissue repair. PRP is particularly popular for tendon injuries, mild arthritis, and sports-related joint damage.
Stem Cell Therapy goes a step further. Rather than relying on growth factors alone, it introduces the actual building blocks the body uses to create new tissue. This makes it one of the most promising frontiers in joint pain management today.
How Stem Cell Therapy Works for Joint Pain

Stem cells are unique because they have the ability to develop into many different types of specialized cells, including cartilage cells, bone cells, and connective tissue cells. In the context of stem cell therapy for joints, this ability is put to work repairing damaged structures that the body can no longer fix on its own.
The most common sources of stem cells used in joint treatment are:
Bone Marrow: Extracted typically from the patient’s hip bone, bone marrow contains mesenchymal stem cells that are well-suited for orthopedic repair.
Adipose (Fat) Tissue: Fat cells are rich in regenerative stem cells and can be harvested with minimal discomfort through a small liposuction procedure.
Umbilical Cord: Cells derived from donated umbilical cord tissue are ethically sourced, highly potent, and don’t require a harvesting procedure from the patient.
Once stem cells are collected and (in some cases) prepared in a lab, they are injected directly into the damaged joint. There, they get to work reducing inflammation, signaling the surrounding tissue to heal, and in some cases, generating new cartilage where old cartilage had worn away.
The process is typically done on an outpatient basis. Patients go home the same day and, over the weeks and months that follow, many report a gradual but meaningful reduction in pain and improvement in movement.
Cellular Therapy for Pain Management
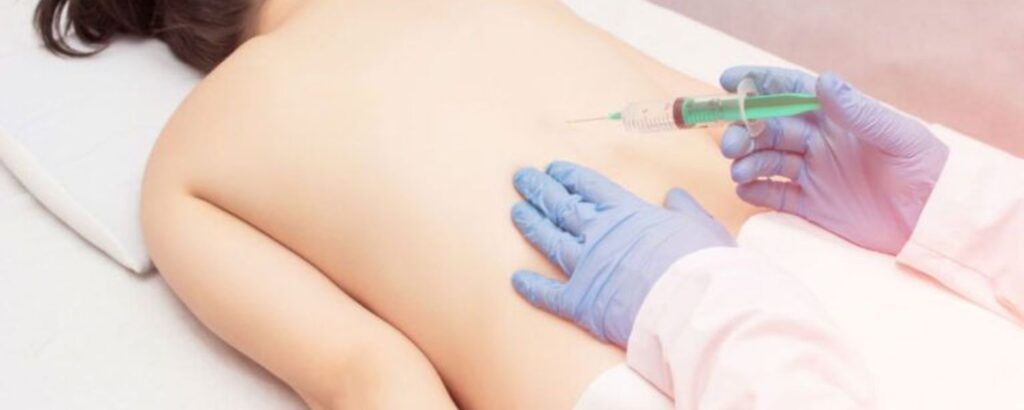
Cellular therapy is a broader term that covers treatments using living cells to restore normal function in damaged or diseased tissue. While stem cell therapy is one form of cellular therapy, the field also includes treatments using immune cells, exosomes (tiny particles released by stem cells), and other biological agents.
For joint pain specifically, cellular therapy is valuable because it targets the source of the problem rather than just its symptoms. Inflammation is calmed at a biological level. Damaged cartilage receives signals to regenerate. The joint environment shifts from one of breakdown to one of repair.
This approach is particularly promising for patients with moderate arthritis who haven’t yet reached the point of needing joint replacement surgery. Cellular therapy may give those patients years of improved function without the risks and recovery time associated with major surgery.
Stem Cell Shoulder Treatment: A Closer Look

The shoulder is one of the most mobile joints in the body, and that mobility makes it one of the most frequently injured. Rotator cuff tears, labral damage, and degenerative arthritis of the shoulder are common conditions that cause persistent pain and limit arm movement.
Traditional treatments for shoulder pain include physical therapy, cortisone injections, and, in more severe cases, surgery. But stem cell shoulder treatment is emerging as a compelling middle ground, especially for patients with partial tears or early-to-moderate arthritis who want to avoid surgery if possible.
In a typical stem cell shoulder treatment session, cells are harvested from the patient’s bone marrow or fat tissue, processed, and then precisely injected into the shoulder joint under imaging guidance. The goal is to deliver the cells exactly where they are needed most.
Many patients who have undergone this treatment report reduced pain, improved range of motion, and a return to activities they had given up, often within two to six months of the procedure.
How Stem Cell Therapy for Joints Can Restore Mobility
Mobility isn’t just about walking or running. It’s about being able to reach for something on a high shelf, kneel to play with your kids, or simply roll over in bed without wincing. Joint damage affects all of these things.
Stem cell therapy for joints helps restore mobility through several mechanisms. It reduces chronic inflammation, which is often the biggest driver of stiffness and limited movement. It encourages cartilage regeneration, which means the joint has a smoother, better-cushioned surface to move on. And it supports the repair of surrounding soft tissue, like tendons and ligaments that may have been strained or partially torn.
The result, for many patients, is a joint that works closer to how it was designed to work rather than one that has to be worked around.
What to Expect During Your Joint Pain Treatment
If you’re considering any form of joint pain treatment, whether regenerative or conventional, here’s a general sense of what the process looks like:
Initial Consultation: A thorough evaluation of your medical history, symptoms, and imaging (X-rays or MRI) helps determine the extent of the damage and the most appropriate treatment path.
Treatment Planning: Your care team will outline the recommended approach, expected outcomes, and what the recovery process looks like for your specific case.
The Procedure: For regenerative treatments like PRP or stem cell therapy, the procedure is typically done in a clinic setting and takes a few hours at most. Most patients feel minimal discomfort.
Recovery: There may be some soreness in the days following an injection, but most patients return to light activity quickly. Full results from regenerative treatments typically develop over several months.
Follow-Up: Ongoing check-ins allow your care team to monitor progress and adjust the plan if needed.
The Future of Joint Pain Treatments
Research into joint pain management is moving quickly. Scientists are exploring ways to make stem cell therapies more targeted and effective, developing new biomaterials that support cartilage growth, and using artificial intelligence to better predict which treatments will work best for which patients.
Gene therapy is also on the horizon, with early research looking at ways to switch on the body’s own repair genes within damaged joints. Exosome therapy, which delivers healing signals without using whole cells, is another area gaining momentum.
The overall direction is clear: treatment is moving away from surgery and symptom management and toward genuine biological repair. For people living with joint pain today, this means the options available are better than they’ve ever been, and they’re only getting better.
Conclusion: Take the First Step Today
Living with joint pain is exhausting. It wears on you physically and emotionally. But it doesn’t have to be permanent.
Whether your pain is in your knees, shoulders, hips, or back, whether it’s been bothering you for months or years, there are treatment paths available that are worth exploring seriously. From regenerative medicine for joint pain to targeted stem cell shoulder treatment, today’s options go far beyond just managing discomfort.
The most important step is the first one: talking to a qualified healthcare professional who can assess your situation and help you understand what’s possible. Don’t wait until the pain forces you into surgery or forces you out of the activities you care about.
Your mobility matters. Your quality of life matters. And with the right joint pain treatment, there’s a real chance to get both back.
Frequently Asked Questions
1.What causes joint pain?
A. Joint pain can result from injury, overuse, arthritis (both osteoarthritis and rheumatoid arthritis), inflammation, infection, or autoimmune conditions. Age-related wear and tear is one of the most common causes, particularly in the knees, hips, and spine.
2. How does stem cell therapy help with joint pain?
A. Stem cell therapy introduces regenerative cells directly into the damaged joint. These cells help reduce inflammation, promote the growth of new cartilage, and support the repair of surrounding soft tissue, addressing the underlying damage rather than just covering up the pain.
3. What are the benefits of regenerative medicine for joint pain?
A. Regenerative medicine offers the potential for longer-lasting relief compared to conventional treatments. It aims to repair tissue rather than simply suppress pain, which means many patients experience improved mobility and reduced dependence on medication.
4. Is stem cell therapy safe for joint pain treatment?
A. When performed by qualified medical professionals using proper protocols, stem cell therapy is generally considered safe. Because most procedures use the patient’s own cells, the risk of rejection or adverse reaction is low. As with any medical procedure, it’s important to consult with a specialist to understand whether it’s right for your specific condition.