Introdution
Chronic pain affects hundreds of millions of people worldwide. Whether it comes from worn-out joints, old sports injuries, arthritis, or nerve damage, the impact on daily life can be devastating.
Simple tasks like climbing stairs, carrying groceries, or even sleeping through the night become enormous challenges. For many people, the standard answer has been a lifetime of painkillers, cortisone injections, or eventually surgery — none of which actually fix what’s broken.
That’s why more patients and doctors are turning their attention to regenerative medicine, and specifically to cellular therapy for pain. This approach doesn’t just mask discomfort. Instead, it works with the body’s own biology to support real healing from the inside out.
As interest in non-surgical orthopedic solutions grows, cellular therapy is emerging as one of the most promising options available to people suffering from long-term pain.
Understanding Chronic Pain and Its Causes
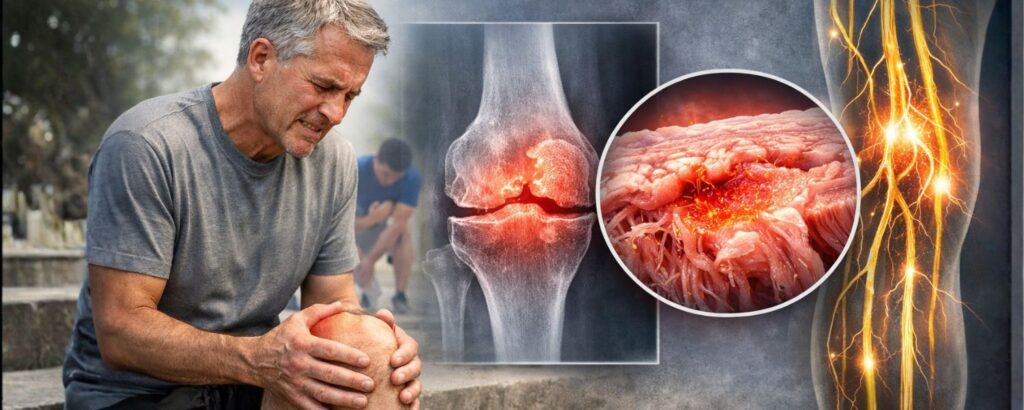
To understand why cellular therapy matters, it helps to first understand why chronic pain is so stubborn and why traditional treatments often fall short.
Chronic pain usually develops when tissues in the body — cartilage, tendons, ligaments, nerves, or bone — become damaged faster than the body can repair them. This can happen gradually through aging and daily wear, or more suddenly through injury or overuse.
Joint degeneration is one of the most common culprits. As cartilage breaks down, bones begin to grind against each other, triggering inflammation and pain. Inflammation itself becomes a self-reinforcing problem — it damages tissue, which creates more inflammation, which causes more damage.
Nerve irritation adds another layer of complexity. When nerves are compressed or injured, they can send pain signals even when there’s no active threat to the body. This is why some people still hurt long after an injury has technically “healed.”
Sports and repetitive strain injuries often cause microscopic tears in tendons and ligaments that never fully recover. Aging-related degeneration slows the body’s natural repair systems, meaning damage accumulates faster than it can be addressed.
The result is reduced mobility, disrupted sleep, mental fatigue, and a significant drop in quality of life. Traditional pain management typically focuses on reducing symptoms — blocking pain signals or dampening inflammation temporarily — without addressing the structural damage underneath.
What Is Cellular Therapy?
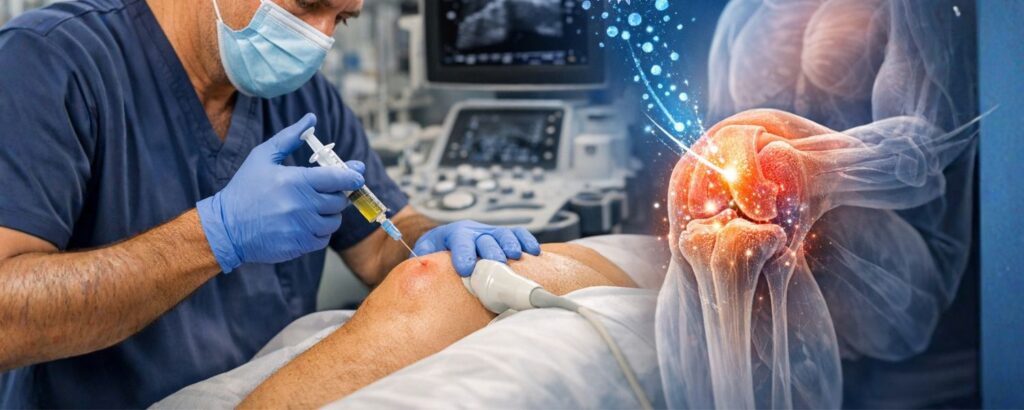
Cellular therapy is a branch of regenerative medicine that uses biological materials to support the body’s own healing systems. Rather than blocking pain or removing damaged tissue surgically, the goal is to encourage the body to repair and regenerate damaged structures.
At its core, regenerative medicine is based on a straightforward idea: the human body already knows how to heal. After a cut, the skin grows back. After a broken bone, new bone forms. Cellular therapy attempts to amplify this natural process in areas where it has slowed down or become overwhelmed.
Regenerative cells play a central role in this process. These cells have the ability to differentiate into various tissue types and release signaling molecules that coordinate healing responses. When introduced into damaged areas, they can help reduce inflammation, stimulate the production of new tissue, and support the repair of structures that the body has struggled to fix on its own.
There’s an important distinction here between symptom management and regenerative healing. A painkiller changes how you perceive pain. A cortisone injection reduces inflammation temporarily. Cellular therapy, on the other hand, aims to actually change the condition of the damaged tissue — not just the experience of it. This is what makes regenerative pain therapy a fundamentally different category of treatment.
How Cellular Therapy Helps Reduce Pain
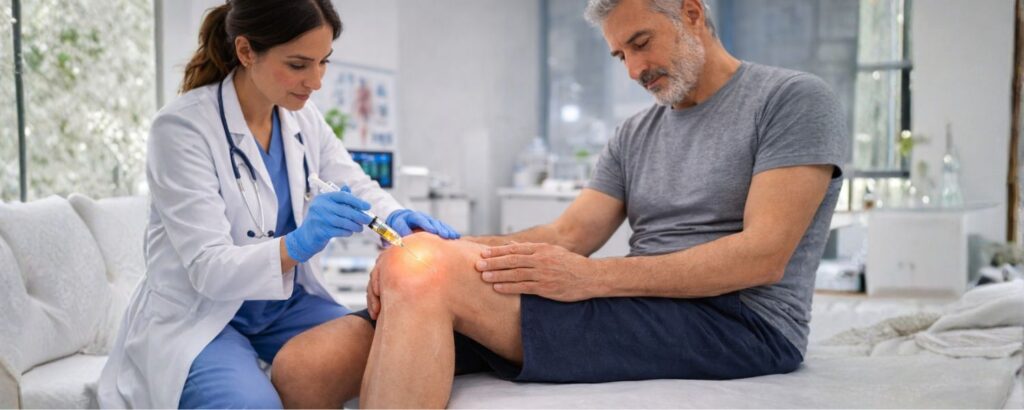
The way cellular therapy addresses pain is closely tied to its effect on the biology of damaged tissue.
When regenerative cells are delivered to an injured area, they release anti-inflammatory compounds that interrupt the cycle of chronic inflammation. This alone can provide meaningful relief. But the more significant benefit comes from the signals these cells send to surrounding tissues.
Cartilage repair is one area where cellular therapy has shown considerable promise. Cartilage has very little blood supply and essentially no ability to self-repair once damaged. Regenerative approaches attempt to create an environment where new cartilage-like tissue can form, reducing joint friction and improving movement.
Tendons and ligaments can also benefit from the growth-promoting signals that regenerative cells release. This helps restore structural integrity to tissue that has become weakened or scarred.
Beyond repair, cellular therapy supports overall joint function. Patients often report not just less pain, but better range of motion, improved stability, and a greater ability to stay active. The focus is on long-term recovery — giving the body the resources it needs to build lasting improvement — rather than temporary relief that fades once treatment wears off.
Conditions That May Benefit from Cellular Therapy
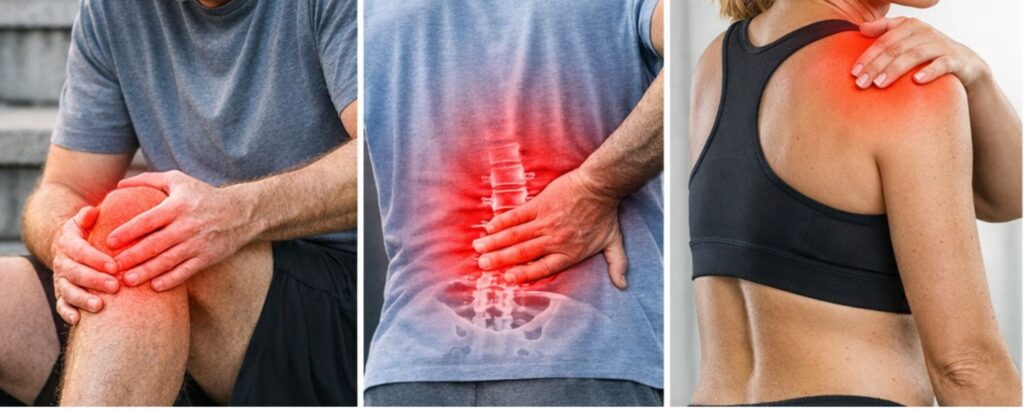
A wide range of pain conditions may respond positively to regenerative treatment approaches.
Knee pain therapy is among the most commonly treated conditions. Osteoarthritis of the knee, meniscus damage, and post-surgical pain are all areas where cellular therapy is being actively explored and applied clinically.
Spinal pain therapy, including degeneration of the intervertebral discs, facet joint arthritis, and chronic lower back conditions, represents another major application. As the discs lose height and flexibility, pain and nerve compression often follow. Regenerative approaches aim to support disc health and reduce inflammation around spinal structures.
Shoulder pain therapy from rotator cuff tears, labral damage, or shoulder arthritis is another common target. These injuries often struggle to heal fully because of poor blood supply and constant mechanical stress, making them good candidates for regenerative support.
Hip pain therapy from arthritis, labral tears, or tendon damage around the hip joint is also being addressed through cellular therapy, particularly for patients who want to avoid or delay hip replacement surgery.
Sports injuries, including damage to the ACL, Achilles tendon, and various muscle-tendon junctions, also represent a growing area of application, particularly among athletes who need to return to high levels of physical performance.
The Cellular Therapy Procedure: What Patients Can Expect
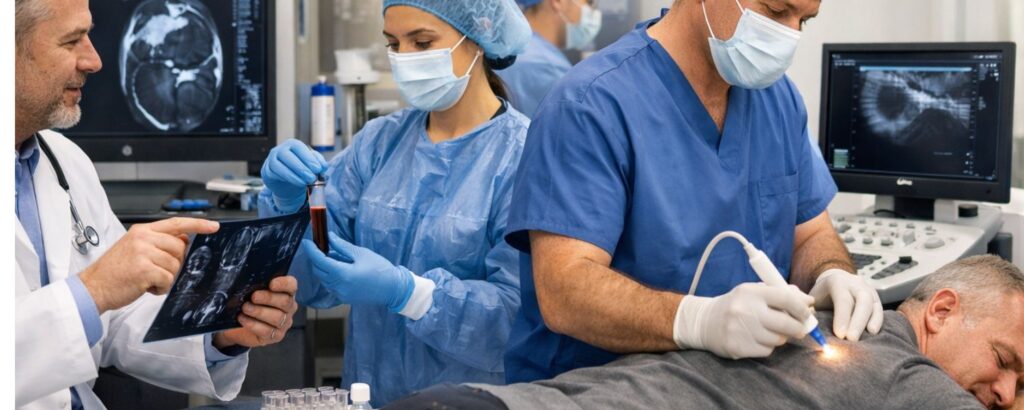
For most people, the idea of a medical procedure brings some degree of anxiety. Understanding the process can help make it feel more approachable.
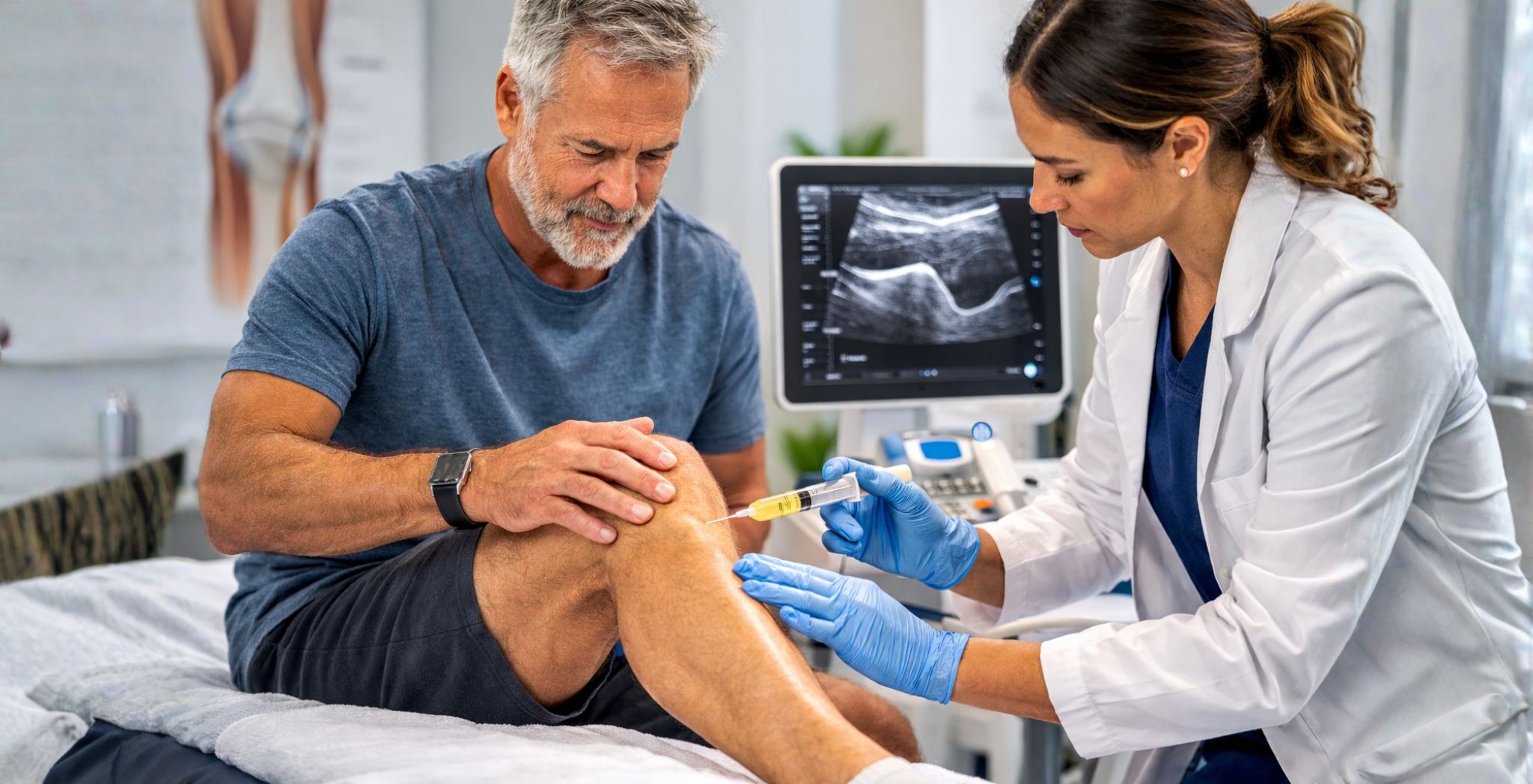
It typically begins with a thorough medical consultation. A specialist will review your history, symptoms, and previous treatments. Diagnostic imaging — such as MRI or ultrasound — is used to get a clear picture of the specific area being treated.
From there, the regenerative materials are prepared. Depending on the approach, these may be derived from the patient’s own body or from carefully screened external sources. The preparation process is conducted under sterile clinical conditions.
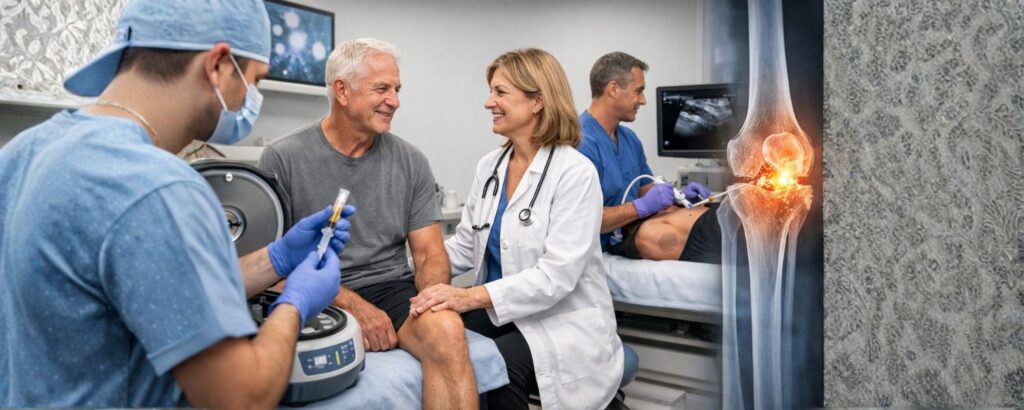
The actual treatment usually involves a targeted injection directly into the affected area, guided by imaging to ensure precise placement. This is typically an outpatient procedure performed in a clinical setting without the need for general anesthesia.
After treatment, patients are monitored and given guidance on recovery. Some degree of temporary soreness or swelling is normal as the body begins its healing response. Most patients return to light activity relatively quickly, with more demanding activities resuming over weeks to months, depending on the individual case.
Benefits of Cellular Therapy for Pain Management

The potential advantages of this approach are compelling, particularly for patients who have exhausted conventional options or who want to avoid surgery.
Cellular therapy is a non-surgical pain management option, which means no general anesthesia, no hospital stay, and significantly lower risk compared to invasive procedures. It supports natural healing rather than working against the body’s own biology. It targets the underlying cause of pain rather than simply covering it up.
Patients who respond well often report improved joint mobility, reduced dependence on pain medications, and the ability to return to activities they had given up. For many, the most meaningful benefit is simply feeling like themselves again — active, mobile, and free from constant discomfort.
Who May Be a Good Candidate for Cellular Therapy

Not everyone is an ideal candidate for regenerative treatment, and an honest evaluation is essential.
People who tend to benefit most include those with chronic joint pain that hasn’t responded well to conventional treatment, patients who want to explore alternatives before committing to surgery, individuals recovering from sports injuries, and those with early-to-moderate degenerative joint conditions.
A professional medical evaluation is essential before proceeding. The right candidate depends on the type and extent of tissue damage, overall health, age, and personal goals. A specialist can assess whether cellular therapy is appropriate and what realistic outcomes might look like.
The Future of Regenerative Pain Treatment
The field of regenerative medicine is advancing rapidly. Clinical research is expanding, techniques are becoming more refined, and our understanding of how regenerative cells behave inside the body is growing with every study.
There is significant interest from orthopedic specialists, sports medicine physicians, and pain management clinicians in integrating cellular approaches into standard care. Non-invasive pain solutions are increasingly in demand as populations age, and the limitations of pharmaceutical approaches become more apparent.
Ongoing clinical studies are exploring new delivery methods, optimized cell preparations, and combinations of regenerative techniques that may enhance outcomes even further. The trajectory of this field suggests that cellular therapy for pain will become increasingly mainstream over the coming decade.
Conclusion
Chronic pain doesn’t have to be a permanent sentence. Cellular therapy for pain represents a genuine shift in how medicine approaches healing — moving away from symptom suppression toward supporting the body’s own remarkable capacity to repair itself. Whether you’re dealing with joint degeneration, a lingering sports injury, or pain that conventional medicine hasn’t been able to resolve, regenerative pain therapy offers a scientifically grounded, non-surgical path worth exploring. As always, the first step is a conversation with a qualified specialist who can evaluate your specific situation and help you understand whether this approach is right for you.